Pediatric variegate porphyria: cutaneous clues to a hidden metabolic disorder
This article has been accepted for publication and has undergone a full review, but has not gone through the editing, layout and proofreading process; there may therefore be differences between this version and the final one.
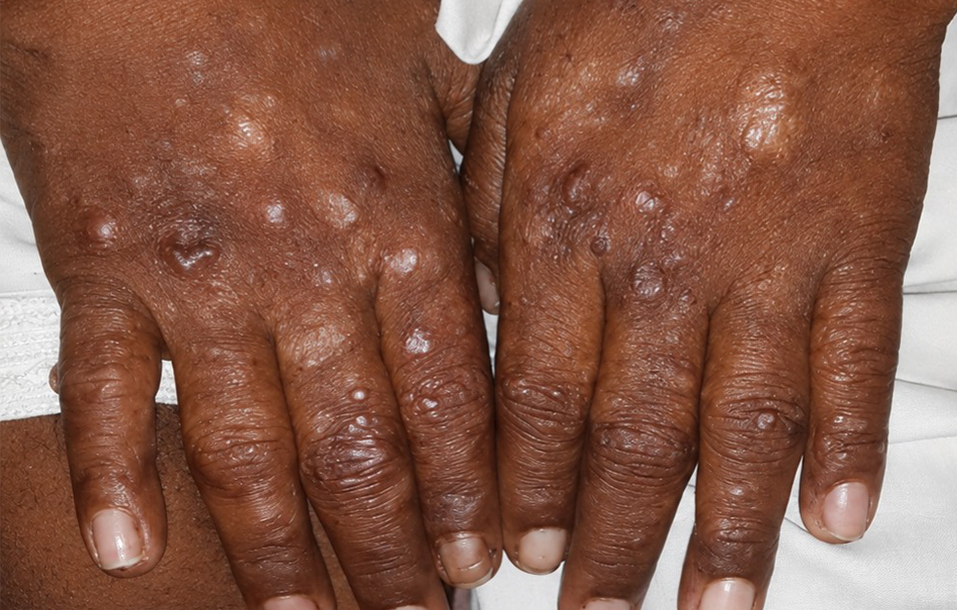
Fig. 2: Variegate porphyria in a 12-year-old boy: scars on the back of the hands.