Multiple pilomatrixomas.
Downloads
DOI:
https://doi.org/10.26326/2281-9649.32.1.2302How to Cite
Abstract
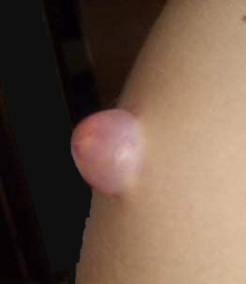
Pilomatrixoma is a benign skin tumor that originates from the outer sheath of the hair follicle. Usually it presents with an asymptomatic, solitary, firm, subcutaneous nodule with bluish-red discoloration of the overlying skin, occurring mostly in the head, neck, or extremities. These nodular tumors are rarely multiple and familial. There is a slight female predilection and it is most commonly seen between the ages of 8 and 13 years old. The incidence of pilomatrixoma is reported to be between 0.001% and 0.0031% of all dermatopathology specimens (4, 5, 6). When examined, pressing on one edge of the lesion causes the opposite edge to protrude from the skin like a ‘teeter-totter”. Also, stretching of the skin over the tumor demonstrates the ‘tent sign’ with multiple facets and angles (2, 4, 5). Definitive diagnosis is performed by biopsy (1). Imaging can be used to rule out blood or lymphatic vascular lesions, ultrasound being the most requested method (1, 2, 4). Ultrasound can help correctly diagnose lesions preoperatively in 76%-95% of cases compared to 33% when the diagnosis is made clinically (3, 5).
As to treatment, surgical excision is the treatment of choice as spontaneous regression of pilomatrixomas has never been observed. Recurrence after surgery is reported between 2% to 6% (5).
Malignant transformation, despite rare, can occur. Pilomatrixomas that are likely to undergo malignant transformation have a higher degree of cellular pleomorphism, high mitotic rate and atypia, central necrosis, and more extensive infiltration into the skin, soft tissue, and blood and lymphatic vessels. Some studies suggest multiple pilomatrixomas association with syndromes such as Gardner, Turner, Rubinstein-Taybi, Sotos and Stickler. These syndromes should be ruled out thanks to clinical features and genetic analysis (4, 5).
