Atrophic vascular patch: early involuting fetal hemangioma?
Downloads
DOI:
https://doi.org/10.26326/2281-9649.31.4.2291How to Cite
Abstract
Regression of infantile hemangioma – IH –, especially when there is a superficial, red component with clear limits, is associated with atrophy of the skin and subcutaneous fat tissue, more often evident on palpation with a decrease in consistency and thickness, but sometimes detectable on inspection with cigarette paper skin. In addition to IH this residual atrophy is present in other vascular proliferations, such as congenital hemangioma – CH – and minimal growth reticular hemangioma – MGRH – (1).
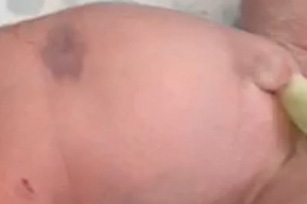
The lipoatrophic lesions of the actual report do not have the characteristics of IH, CH and MGRH. Clinically, they are vascular lesions due to the red or bluish color, sometimes due to the presence of an ischemic halo, and in other cases due to the presence of telangiectasias on dermoscopic examination. In favor of the hypothesis of a rapidly regressing fetal hemangioma is the progressive clearing of the lesions over the months. Due to the modest size of the lesions and the progressive clearing they undergo, it is less likely that they are malformative vascular lesions, although in the literature there are reports of lipoatrophy associated with vascular malformations (2, 8).
It is possible that to determine the lipoatrophy is the same hypoxia that is responsible for hemangioma and that would inhibit the lipogenesis and differentiation of adipocytes (1). In the cases described in the current report, there are no prematurity, pregnancy or perinatal changes, which are known factors favoring IH. It is possible that a minimal and reversible arterial alteration is responsible for hypoxia. The relationship between arterial hypoxia and hemangioma has been repeatedly reported in the literature, especially but not only in the PHACE and PELVIS syndromes; you can think of the hemangiomas associated with Poland syndrome (7), the absence of the carotid artery (6), and vascular anomalies with acral defects of the limbs (3). In 2008 Mazzotta et Al. (4) described cases of minimal growth, segmental hemangiomas of the lower limb that underwent ulceration in the 7-8 month of age and in one of these cases they documented an iliac artery malformation as responsible for ulceration. Other Authors emphasized the relationship between minimally growing hemangiomas, ulcerations and arterial malformations, such as ectasia of the common iliac artery and hypoplasia of the femoral artery (5). In case 1 of the report by Bessis et Al. (1) a focal lipoatrophy is present in a minimal growth reticular hemangioma of the thigh that undergoes an unusual ulceration both for location – outside the diaper –, and especially for the time of onset – in the seventh month of life – and which could therefore be linked to an arterial anomaly.
