Microsporic kerion followed by dermatophytide and later by Koebner-psoriasis.
Downloads
DOI:
https://doi.org/10.26326/2281-9649.29.3.2018How to Cite
Abstract
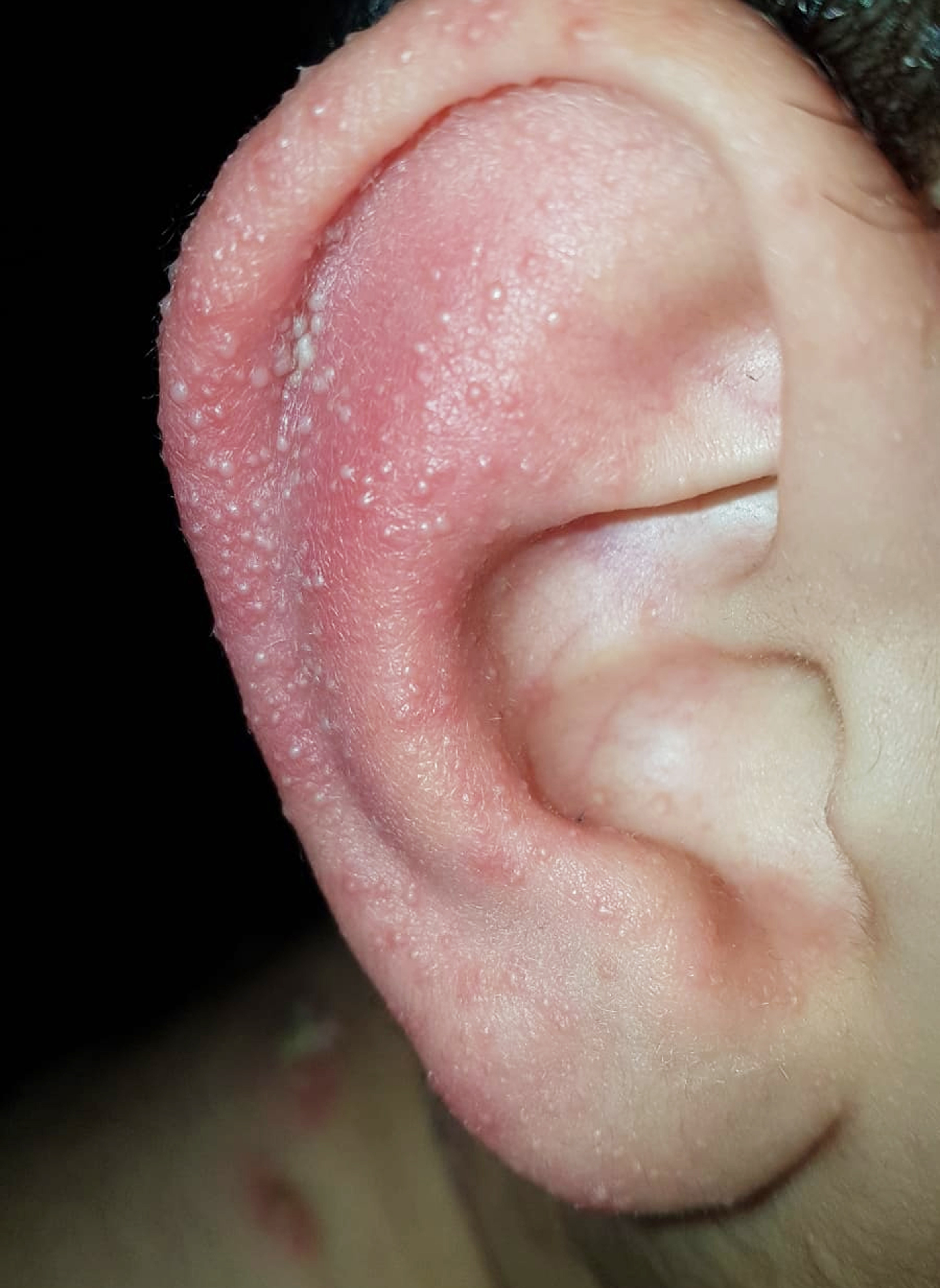
The actual case is interesting for two reasons: the appearance of a self-healing micro-pustular eruption immediately after the beginning of therapy and the onset of psoriasis in the same site of kerion after a few months. The incidence of allergic reactions to fungal antigens varies widely according to the different Authors and the different criteria adopted for the diagnosis (2). For the diagnosis of dermatophytide the following criteria should be met: a- causal fungal infection demonstrated with mycological examination, especially when unilateral (for example of a single foot in the case of pompholix of the hands secondary to tinea pedis); b- secondary lesions morphologically of various type but bilateral and symmetrical (for example of both palmar regions in case of pompholix) with negative mycological examination and positive cutaneous allergological tests to fungal antigens; c- spontaneous resolution of lesions when causal infection stops. From the morphological point of view the causal lesions are characterized by intense inflammation; not by chance the first dermatophytide was described by Jadassohn in a kerion. The secondary lesions can be of various type, but mainly eczematous, papular and pustular (2); they may occur before starting therapy or immediately after starting treatment. The ides of the second case are probably linked to the massive destruction of fungi and are reminiscent of what happens in syphilis with the Jarisch-Herxheimer reaction or in onchocerchiasis and other parasitoses after treatment with albendazole or ivermectin with the Mazzotti reaction (1).
The knowledge of the ide reactions that arise after the beginning of the therapy is important from the practical point of view because the suspicion of an allergic reaction to griseofulvin could lead to drug withdrawal. When the drug, for example griseofulvin, has never been taken before and the ide reaction occurs within 5-6 days from the beginning of the therapy, it is possible to exclude an immune mediated reaction to the drug because the minimum time for a first sensitization to be realized is 7 days.
Also interesting in the current case is the appearance of psoriasis on previous kerion that recalls the phenomenon of Koebner and occurred in a subject with positive biparental family history for psoriasis.
