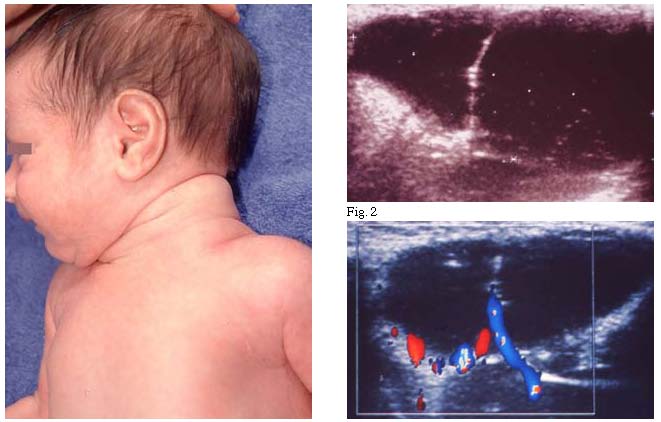
Cystic hygroma
Downloads
DOI:
https://doi.org/10.26326/2281-9649.27.3.1469How to Cite
Abstract
Cystic hygroma is a cavernous deep lymphangioma characterized by the presence of few large cystic cavities often separated by a dense fibrous septum. The most characteristic localization of the neck seems to be related to the presence of a large lymph sac in the neck at the side of the jugular veins in which the main lymphatic ducts – the right and the thoracic ducts – flow into the venous system. It has been hypothesized that the cystic hygroma derives from a faulty communication between the lymphatic ducts and the venous system (1). Lymphangiomas are clinically characterized by periodic variations in volume and color generally related to intralesional bleeding or displacement of lymph from one compartment to another (6). Intralesional hemorrhages should not be surprising when considering that very often malformations of lymph vessels are associated with malformations of blood vessels. Clinical variations are so important that a deep lymphangioma can only become clinically apparent when an intralesional haemorrhage occurs and disappears again when the bleeding is reabsorbed. In our case, the swelling that occurred in the 15 years 4 times, at birth, at 3, 8 and 15 years, was never associated with clinical evidence of intralesional bleeding, so it can not be explained by this mechanism. Another clinical feature of lymphangioma is that it is not a cellular tumor such as infantile
hemangioma but rather a complex vascular malformation with poorly defined limits: this causes the surgical removal of a lymphangioma to be particularly difficult and often followed by recurrences (2, 4). For this reason many Authors believe that the elective therapy of cavernous lymphangioma is sclerosing. The latter can be performed with doxycycline (3), bleomycin (5) but above all with picibanil (OK-432) which is a lyophilized group of Group A Streptococcus pyogenes.
Taking into account the frequency of recurrences and the spontaneous reduction of many lymphangiomas that become clinically relevant only after exceptional traumatic events, therapeutic interventions should only be carried out in case of compression of vital organs and significant esthetic damage, in the latter case after a long period of clinical observation aimed at evaluating possible spontaneous regression (6), sometimes definitive (8).
