Allergic contact dermatitis to topical excipients of propranolol.
Downloads
How to Cite
Foti C., Bonifazi E. 2014. Allergic contact dermatitis to topical excipients of propranolol. Eur. J. Pediat. Dermatol. 24 (2):122-23.
pp. 122-123
Abstract
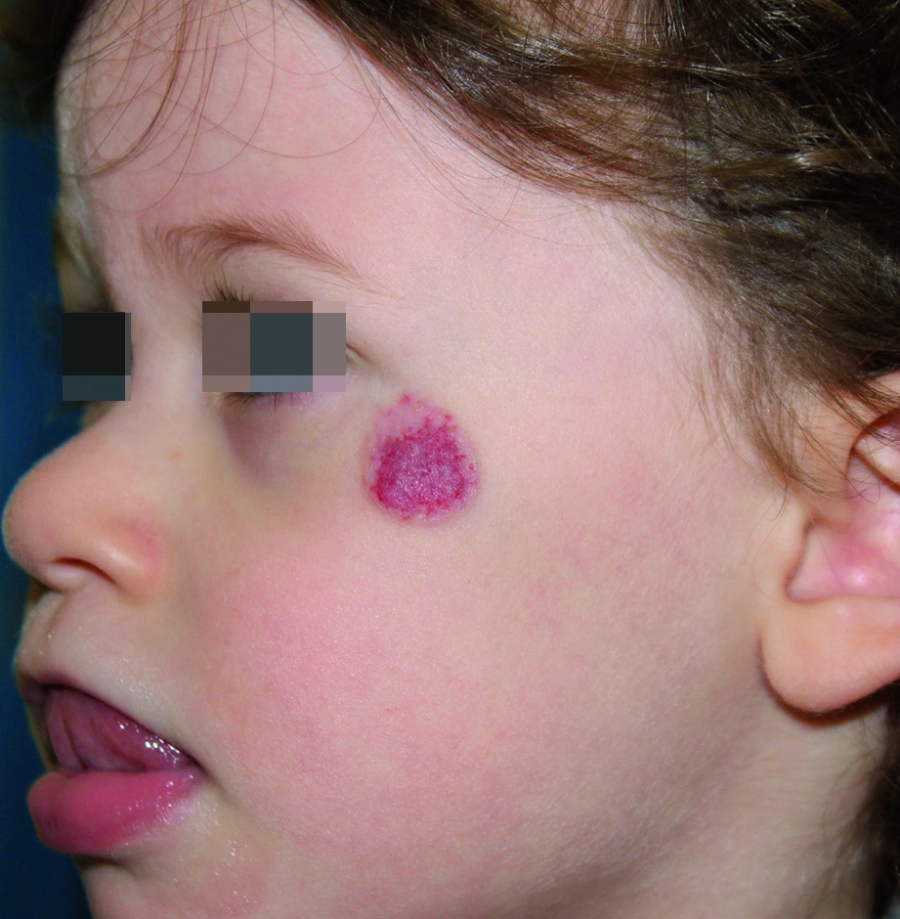
Case report. A 3-month-old little girl started oral propranolol at a dose of 2 mg/kg per day for a periocular hemangioma (Fig. 1). The hemangioma improved by 60% (Fig. 2) and 9 months later the therapy was discontinued. At the age of 2 years, the superficial component was still evident (Fig. 3). Therefore, she started 1% topical propranolol twice a day. After 2 months of therapy the mother called us alarmed because the hemangioma had suddenly reddened, swollen and covered with scales. We recommended to discontinue propranolol and apply a topical steroid. When we saw the baby after 2 days hemangioma was still red and swollen (Fig. 4). The child was not affected by atopic dermatitis. However, to be certain of the role of the cream we advised to apply the topical propranolol on her left wrist. 2 days later papules and vesicles appeared on the wrist (Fig. 5), while the hemangioma returned to the "status quo antea" (Fig . 6). 1 month later the patch tests were negative for timolol, propranolol in water and vaseline, but positive for the cream used by the child which contained elfakos, cetamacrogol, cetearyl alcohol, glycerin and almond oil. The final diagnosis was allergic contact dermatitis to excipients. Patch tests with the individual components were programmed and topical propranolol in petrolatum was continued, without causing any problem to the child.Keywords
Allergic contact dermatitis, Topical excipients
